| You are here: Home: BCU 9|2003 - Supplement : Case 7: From the practice of Gregory R Favis, MD
| Case 7: From the practice of Gregory R Favis, MD |
- 76-year-old woman with a T3N1, ER-negative, PR-positive infiltrating ductal carcinoma in 1991
- Treated with mastectomy and reconstruction, radiation therapy, AC x 4, tamoxifen x 5 years
- Seven years later, relapsed in the skin and subcutaneous tissue (ten 1-cm lesions), metastatic work-up negative, otherwise asymptomatic
- Received an aromatase inhibitor, progressed within three months
- Lesion rebiopsied: ER-negative (similar histology to original tumor)
- Received capecitabine/docetaxel x 3 cycles: Minimal response and docetaxel discontinued
- Continued capecitabine: 50 percent response, remains on capecitabine for 18 months with no evidence of disease progression
|
Dr Favis: This 76-year-old woman had a T3N1 ER-negative, PR-positive breast tumor in 1991. She was treated with a mastectomy, AC for four cycles, radiation therapy and then tamoxifen for five years.
Seven years later, she relapsed in the subcutaneous tissues. She was started on an aromatase inhibitor and progressed in three months. We went back and rebiopsied one of the skin lesions, which we didn't do initially because it's so usual that somebody with such a long progression will have an ER-positive tumor. But we went back and rebiopsied one of these lesions, which was ER-negative.
Dr Love: Could you describe where these skin lesions were and what condition the patient was in?
Dr Favis: She was actually in pretty good condition. She and her husband were long-distance truck drivers, and she would go with him for two weeks at a time. She had been able to do that all along, so her performance status was completely normal. As for the skin lesions, there were about 10 of them, all about one centimeter in size but diffusely scattered over the back of her ears and her back. They weren't really bothering her, other than she knew they were there and they were slightly pruritic. There was no evidence of visceral organ involvement or other metastases in her work-up.
Dr Love: And so her original ER was in 1991, and that was ER-negative, PR-positive?
Dr Favis: Right.
Dr Love: And then you repeated it on the biopsy and it looked histologically like the same tumor?
Dr Favis: Yes, as best as we could tell.
Dr Love: The other breast was normal - no evidence of a new primary cancer?
Dr Favis: Correct. Her mammogram was negative.
Dr Love: You mentioned that she's a truck driver and she wanted to continue being able to take off for a couple of weeks at a time with her husband. Was this for personal or financial reasons, or both?
Dr Favis: Financially, it was not an issue. She just enjoyed going with him and it was part of their life together.
Dr Love: What was her reaction when she first was diagnosed with metastatic disease? How did she cope with that?
Dr Favis: I think women who have had breast cancer are always waiting for the other shoe to drop, so it wasn't that big of a surprise. But it had been 12 years since her initial diagnosis. She handled it well. A lot of people have blind faith that we can cure anything, and she kind of had that same feeling. I wish I had the same feeling.
Dr Love: To what extent were these skin lesions bothering her?
Dr Favis: They were starting to bother her cosmetically. That was her main concern.
Dr Love: Lisa, how would you have thought through this situation? This woman had prior AC 12 years ago, along with postmastectomy regional radiation therapy. She apparently has an ER-negative tumor with these skin lesions. What would you be thinking in terms of treating this 76-year-old woman?
Dr Carey: I think the first thing is that you probably can be somewhat reassuring by telling her that women who relapse after such a prolonged disease-free interval tend to live for a long time, and their disease tends to be easier to treat or at least more indolent.
Regarding her treatment options, she has an active lifestyle; she's asymptomatic and wants to be able to leave town for a couple of weeks at a time. I think you can give her something that's likely to have low toxicity - perhaps capecitabine. I wouldn't give her the full dose, if you're trying to avoid toxicity. You can also consider paclitaxel.
Dr Love: Dr Favis, since Lisa mentioned capecitabine, how did you think she would be in terms of compliance? Did you think she would have reported back symptoms and taken the drug reliably.
Dr Favis: Yes. Absolutely. She was a really excellent patient in that regard.
Dr Love: Lisa, is that an important factor when you consider capecitabine?
Dr Carey: Absolutely. With any oral drug, you have to have a strong relationship with the patient and know that they're going to take it reliably and report back to you.
Dr Love: Peter?
Dr Ravdin: This is a case that Craig Allred would love. He would predict that this case would be ER-positive, even after hormone therapy failed. And so I guess one of the things I would do is retest her ER status. And I would consider, possibly going back and using tamoxifen, because there's something odd about this case with the very late recurrence.
Dr Love: Let's say you send the tumor to Craig Allred and he says, "It's absolutely zero. I don't see one ER-positive cell there." Would you still try a hormone?
Dr Ravdin: It's not out of the question. This is the kind of patient who's going to have a long, slow progression and I would certainly think about it.
The other question I might ask -because we've all seen these patients, and there's no special reason why it seems to happen - is whether she's taking some root preparation or some other unconventional therapy. I'm always curious as to why somebody would develop multiple metastatic sites of disease 12 years after the fact.
Dr Love: Any suggestion of alternative approaches here?
Dr Favis: No. But she had reconstructive surgery and I've seen some peculiar patterns of recurrence after reconstructive surgery. One of the sites of recurrence initially was right at her suture line.
Dr Love: What happened with this lady?
Dr Favis: When she didn't respond to
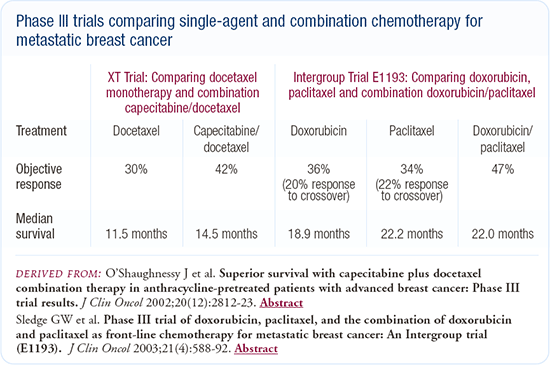
the aromatase inhibitor, it was roughly at the time during which Joyce O'Shaughnessy was talking about the capecitabine-docetaxel data (Figure 7.1), and so I decided to try her on that, even though she didn't seem very symptomatic. She went through three cycles of the docetaxel, and I really wasn't impressed by the response. These things are difficult because when you have a lot of subcutaneous things to measure, they're hard to quantitate. There didn't seem to be much of a response, so I left her on the capecitabine and she has had, I would say, about a 50 percent response. She's still on the capecitabine at 18 months and hasn't recurred in any other site. She likes the capecitabine because she can take it when she goes with her husband, and she's still out trucking with him.
Dr Love: How did you start the dosing and have you had to modify it?
Figure 7.1
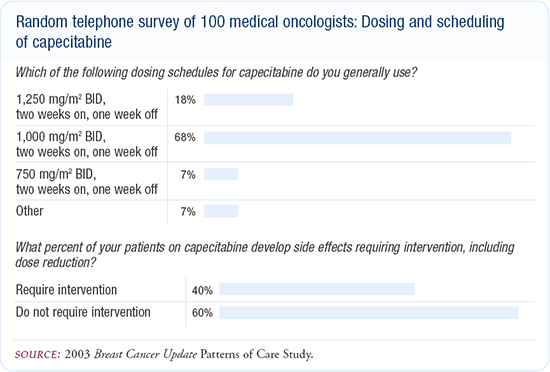
Dr Favis: I started at close to 2 g/m2 per day in two divided doses for 14 days on with seven days off, and I've had to dose-reduce a little bit because of hand-foot syndrome, but not much (Figure 7.2).
Dr Love: It's interesting that in our patterns of care surveys, one of the things that we consistently observe in both community physicians and research leaders is that frequently they start their patients with ER-positive tumors on chemotherapy, and then, after the patient stabilizes, they switch to hormonal therapy. I've also heard about the strategy used in this case, in which you start off using the combination of capecitabine and docetaxel and then continue the capecitabine - sort an induction-maintenance approach. We presented a case like this to Joyce O'Shaughnessy at the last Miami Breast Cancer
Conference and that was how she approached the patient. Lisa, is that a strategy you've used in your practice?
Dr Carey: Yes. I think, for the symptomatic patients, that's typically what we would do - use a combination. For someone who comes in with a lot of disease, use the combination to obtain the best response you can, but then continue them on something much less toxic as a single agent. If they've responded to the combination, we make our best guess as to which agent was the most important and most tolerable, and then continue with that. I'd say that's actually a very good paradigm.
From the floor: I was wondering, in a case like this where you have a 12-year, disease-free interval, would the histological grade on that biopsy help you? Let's say you found that it was a very well-differentiated tumor. Even if the tumor was ER/PR-negative, would you be more apt to think it was positive and treat it as such?
Figure 7.2
Dr Love: Peter, that relates to what you were saying.
Dr Ravdin: I think you have nothing to lose by trying a hormone in a patient with indolent disease, and there are documented responses. There are clearly patients in whom the antibody doesn't pick up the fact that they have a functional estrogen receptor. Particularly in this case, to give it another spin would certainly be reasonable.
From the floor: There are clinical trials for first-line therapy in metastatic disease that should also be considered for a patient to enter. There's an ECOG study of paclitaxel plus or minus bevacizumab (Figure 7.3). It's an interesting study because second-line bevacizumab didn't work with
capecitabine, but this is an ECOG first-line trial, and we'll see what happens. I have had patients on that trial and it's a relatively easy regimen for the patient.
From the floor: I have a question about the toxicity of the therapies and how much is necessary to obtain a response. I wonder why we subject everyone to the toxicity of the maximum dose of the therapy? I'm a bit of a therapeutic nihilist. I think that quality of life is important, particularly in the metastatic setting where treatment is palliative.
Dr Love: Bob?
Dr Carlson: With many of the agents that we use, including capecitabine, the evidence of a dose-response relationship is very poor. And if there is a dose-response curve, it's very shallow. I think that the FDA-approved dose of capecitabine of 2,500 mg/m2 daily, divided into two daily doses, is much too toxic. I start it at 2,000 mg/m2 divided in two daily doses and, with that, my experience is that you usually end up rapidly dose de-escalating rather than escalating.
Another difficulty with dose escalating capecitabine is that the toxicity experience is often cumulative. If you dose escalate you sometimes think that the toxicity is because of the dose escalation, but it may be a result of the duration that the patient's been on therapy.
Figure 7.3

Select publications
|
